Patient Stories
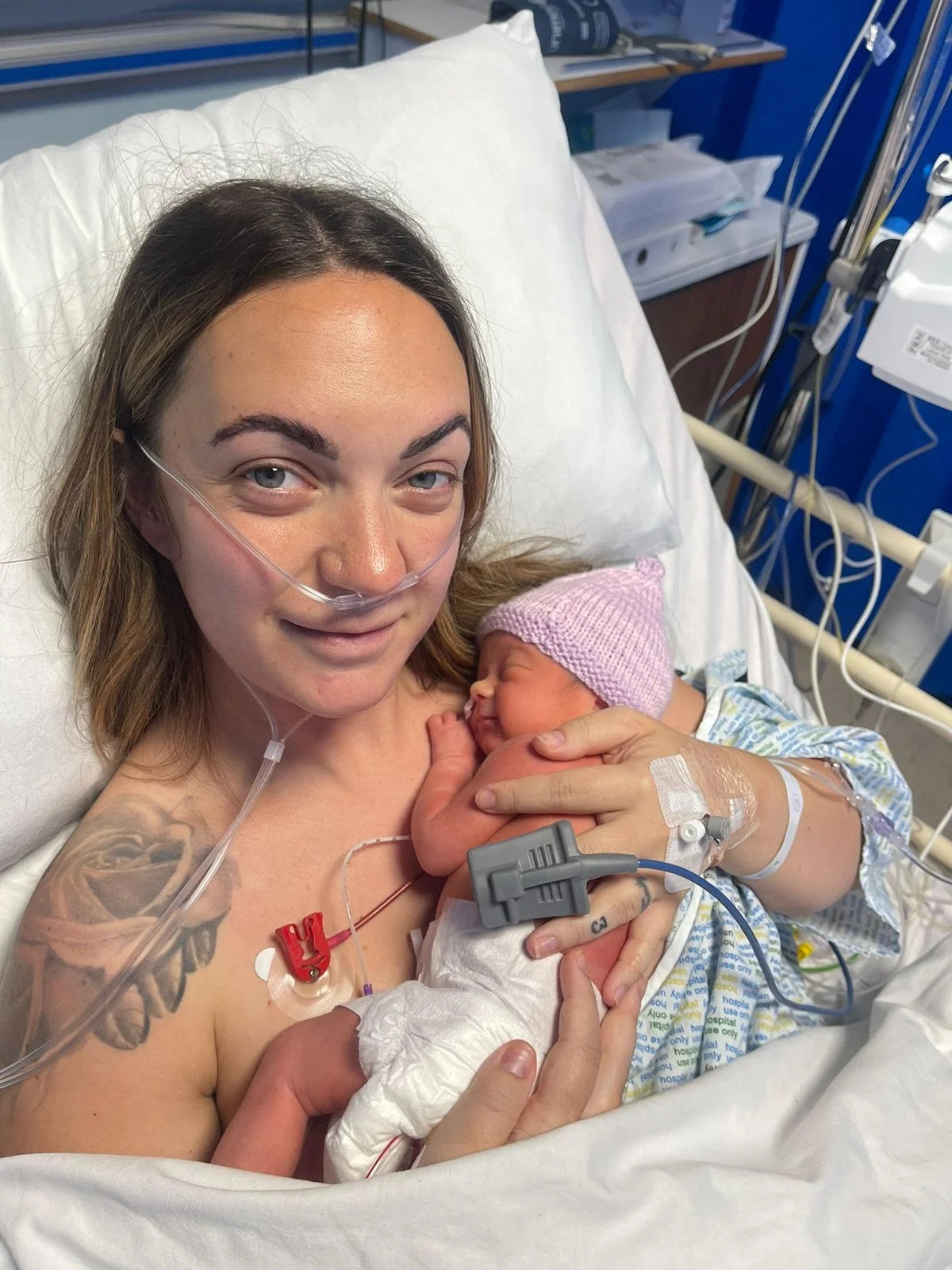

Rachael Murray
Back in October 2024, we were filled with excitement and nerves as we found out we were pregnant with baby number 2. Keeping it all secret from friends and family until it was confirmed "safe" and surprise them. However, two weeks after getting our positive test - I attended Wishaw Early Pregnancy Unit for a scan due to bleeding. They couldn't confirm the pregnancy as it could have been too early or we could have lost already, however with the gestational sac being in a teardrop shape they said it could likely turn into a miscarriage. We had to prepare ourselves for the worst yet hope for the best.
We were asked to return two weeks later for another scan and allow time to see what happens. We had booked for a private scan a week after our first appointment at EPU and instantly confirmed the baby & heartbeat. We couldn't believe it! We were told the baby had implanted lower than "normal “but was told this can happen. Pregnancy symptoms then came charging on and as horrific as I felt it was confirming with myself, we had a strong little one growing. Thankfully the rest of my pregnancy was going well, we hit those milestones of 12weeks, 16weeks and then came 20weeks along in January 2025 when we attended Wishaw once again for anatomy scan. It was here when things started ringing some alarm bells. We decided not to find out the baby's gender however at the very end of our appointment our midwife checked placenta placement and discovered I had placenta previa and a part of my section scan looked "a little funny" so she went to get a second opinion but reassured us everything was ok. A consultant came in to check me and asked us to come back to her clinic the following week, where she would have more time to look and decide what was going on. We were told at the end of the appointment that depending on what she finds the following week we may need to be referred to the specialists in Glasgow, and they can confirm confidently what's going on.
A week later, I attended the clinic and yes there was an issue with my scar tissue and the placenta - no diagnosis or medical term was used. All I was told was she was referring me to Glasgow to the specialists, and they are classed as "placenta people" and if it is what she thinks, it could end in a hysterectomy. I felt like I was stabbed in the chest. Hearing that word, hysterectomy. I was in shock, confused, devastated - how could a 20week scan go from everything is fine with just a little concern with placenta to it might end in a hysterectomy. I was 31. Things like this don’t happen to 31year olds. Myself and mum left the appointment with so much worry, concern, relieved baby was ok and not affected but the uncertainty was horrible. I had to sit and wait on the call from Princess Royal Maternity to go in for a scan & thankfully Dr Marcus McMillan called 2 days later and had us in that very same day at 4pm for a scan. This was then when himself and Dr Rachel Bradknock confirmed Placenta Accreta Spectrum. We were taken into a small consulting room after the scan and Marcus went into explaining what exactly Placenta Accreta Spectrum was. I was told the likelihood of a hysterectomy is high in cases but also, they can't fully confirm until the day of the procedure.
I just remember feeling so devastated, it was so difficult to take in all the information. We had so many questions. All to which they answered the best they could to help us prepare for what was ahead of us. I felt so helpless. I just cried the whole appointment, how were we going to navigate through such a complicated time?! That evening, I went onto social media and searched for Placenta Accreta Spectrum and all the videos were American - which wasn’t the most helpful as a lot of the women didn't know they even had it. On Instagram - I found Placenta Accreta Scotland & Placenta Accreta Ireland and that was the most helpful resource I came across. Emma from Placenta Accreta Scotland responded to my message and added me to a WhatsApp group where only 5 of us were a part of it then, and honestly these girls have been so incredible and played a massive part of our journey. I have vented, asked question after question, messaged at all hours when life was so uncertain. I had many nights not sleeping, my mind was 100mph trying to digest and discover more information on such a serious matter yet completely unknown.
We were now under the care of Dr McMillan and Dr Bradknock and attending more appointments over the remaining course of the pregnancy. Watching the growth of placenta to uterus and other organs to plan more and more for when birth-day was upon us. I stopped working at 30weeks as I was warned to not be alone from 30weeks onwards and they’d likely take me into hospital for the baby's arrival of 34-36weeks. Due to the seriousness of our condition we decided to find out the baby's gender, so we could concentrate on being prepared for our journey through our last pregnancy and recovery. We had a small intimate evening with our immediate family and found out we were having a baby girl. A gentleman's family as some would say. A boy and a girl, our family complete. Fast forward to Easter Sunday 20th April 2025 - after spending the day at my gran's bedside in her final days on Earth, I was back home with Graeme and Rory when I realised I'd been bleeding. Panic and fear set in and we had to call family to come for Rory and fly out the door straight to PRM while calling ahead to let them know. I was assessed instantly, a heartrate monitor on our baby girl and assigned to a bed on the antenatal ward until Dr Bradnock came round and confirmed what I already expected. I was there until after our baby girl’s arrival. Heartbroken, helpless and a little relieved (oddly) I just wanted to be safe and knowing I was in the right place for that was the only thing getting me through.
The following day I was assigned my own private room due to being a long stay patient. It was so isolating, scary, emotional - it was very much a rollercoaster of emotions. I met a lot of the medical team on my stay, everyone who would be involved on the day and that made faces a lot more familiar. I also met with an infant feeding nurse, Tanya, who later would be one of life's true angels. I was determined to breastfeed as I knew our girl would be early and it was a deep determination and passion that I wanted to breastfeed and give her as much goodness and nutrients to help her thrive. Thanks to Tanya, she really made that happen, she also organised us to visit the Neonatal Ward to familiarise ourselves with the ward and prepare ourselves for our time there if our baby girl was needing extra help. I was also assigned a Psychologist, Kirsten, she visited me on the ward once a week to help process our journey so far and that was exactly what I needed. Some days were ok, some were extremely lonely and others were good! Knowing Kirsten was there to listen, not judge, really helped me feel listened to and validated on how I felt in that moment.
I had 2 more small bleeds which would always happen on a Saturday evening, and every weekend was filled with anxiety as I felt like a ticking timebomb... surprisingly enough and unfortunately on Saturday 10th May I had experienced a few cramps but thought nothing of it and went to sleep and hoped it would pass. At 1.30am I was woken by extreme cramps and went to the toilet to only see a lot of blood - I buzzed the nurses as I had done before when this happened and explained. She checked it out and shouted, "straight to labour suite". I was told to get back on the bed, and they were taking me down. Panic and adrenaline kicked in, tears and uncontrollable tremors took over. I was so scared and lonely. They kept me calm and assured me I was in safe hands, my nurses on the labour ward were also fantastic and reassured again that myself and baby were safe. I didn't know whether to call Graeme, is this an emergency? Will my baby girl need to come now? My mind was spiralling. I was given pain meds to help with the pains I was having and things settled. I called Graeme at 5.30am and told him what was going on, we got grandparents for Rory, and he came straight to the hospital. A few hours later and many consultants later it was confirmed that our planned date Friday 16th May would now be getting pulled forward to Monday 12th May2025. We discussed steroid injection for helping baby's lungs to which I agreed with and received those on Saturday afternoon and Sunday afternoon. The bleeding slowed down and eventually stopped on Sunday morning. We met with multiple medic teams to sign all paperwork and consent forms and the nerves and excitement set in as we were just 1 day away from meeting our little girl.
Monday 12th 2025 -35weeks exactly was the day Mabel arrived. We were wheeled down to the theatre 10am and with Graeme by my side, we met all our doctors and nurses, feeling nervous but safe. I had opted for a spinal epidural for the first half of the section as I wanted (if it was safe to do so) to be awake to see our little girl come into the world. Everything went smoothly in the first half of the morning. It was only when the balloon was inserted to my left groin artery that I felt "a tickle to my heart" which made me realise how serious this whole procedure was. That was scary. Thankfully resolved as quickly as it had happened, we were all ok.12.35pm Mabel was born. 4lb13oz.She was perfect. She cried, myself and Graeme cried and she was taken to the NICU team with her dad by her side. They were hoping to bring her back to me, but Dr McMillan said they would need to press on to which I agreed. As long as I saw Mabel here was my main goal and one of our midwives showed me a quick photo of her, I was relieved and nodded to the Drs to continue on. I was then placed under a GA for the rest of the procedure. I later remember waking up in a large recovery room, nurses chatting but I wasn't 100%"with it". They then wheeled me up to HD (high dependency) where I was met with my sister Laura and husband Graeme. I think this was roughly around 5/6pm. I was so happy to see their faces. I don't remember much due to the GA and other pain meds, but I was just happy to be back with Graeme and instantly asked about Mabel. She was doing so well! She was on a cpap machine for an oxygen boost but all her obs were great. Graeme got to go down to visit her often and take Grandparents down to visit her also. My nurses on HD were so incredible, the 1-1 care was so important for my recovery and not just for me but for the support for Graeme too. He stayed by my side every night until I was moved to the postnatal ward 2 evenings later. The following day, Tanya (Infant Feeding Nurse) came to visit as my nurses had been sending down syringes for my expressed colostrum for Mabel and unbeknown to me she brought Mabel with her. Off her oxygen but with a feeding tube I got my first hold of my Baby girl. Overwhelmed with emotion I couldn't believe we were here. So tiny, so perfect taking in everything about her.
Over the 8days prior to our discharge Mabel needed light therapy for jaundice. Mabel had 2nights in NICU and then 2days in special care before I was then discharged by the postnatal ward and moved to the Neonatal Rooming Inn Suite where Mabel was able to be in next to me as medically, we were both well, we just had to establish her feeding and weight gain. Just me and my girl, together. It was so lovely but again so isolating and filled with guilt. How I ached to be home with Graeme and Rory yet knew it just couldn't happen, yet. By Wednesday 21st May we were discharged home as a family of 4. A surreal feeling, to be able to walk out those hospital doors and be free. It was so emotional, leaving our Drs and Nurses who cared for myself and Mabel for so long. We wrote thank you cards for individual nurses and the wards that I attended (which was a lot) as without their care, their support we would have been so lost. Everyone we crossed paths with were incredible, we really can't begin to explain how grateful we are to have them as our team and make this really difficult and traumatising journey a little easier. To have a hysterectomy at 31years old, mum of 2 - I'm ok with that. I had to flip my mindset and say it doesn't matter what organs I have, or whose blood is in my veins, as long as I see my two kids grow up is all that matters. I wasn't upset when Dr McMillan came to tell me the extent of our operation. I was actually glad it had all been taken, other than my ovaries and cervix. I know my body should have worked better but I don't blame it.
Placenta Accreta is a completely unlucky roll of the dice and nothing I could have done could have changed a single thing, and for me I just had to lie down and accept that. I don't wish for this to have happened to anyone, but I feel the women I've met through having PAS and educating many more about it have driven me to share my story. Each one being so unique and it all matters. We are now 7months down the line, Mabel is thriving after a rough couple of months proving to be a little drama queen, but she is the smiliest little girl. Physically I have healed really well, my scar is still a slight trigger for myself which I'm working on with my psychologist. Mentally I have been diagnosed with PND however with everything I've been through and juggling now 2kids and Mabel having colic, reflux, tongue tie etc it's not a shock my mind went a little wobbly. We are working through it all and I really couldn't be more grateful for our medical team and the support from Placenta Accreta Ireland & Placenta Accreta Scotland.
PAS Mum
